You know the feeling: you’re sitting at your desk, driving home, or maybe even lying in bed, and suddenly, the "alarm bells" go off. Your chest tightens. Your breathing gets shallow. Your heart starts to flutter or race.
Logically, you know you are safe. There is no tiger chasing you. But your body is reacting as if you are in immediate danger.
For many people, the scariest part of anxiety isn't the worry itself—it’s the physical symptoms of anxiety. It’s the feeling that your body is "revved up" and out of your control. When these sensations hit, it’s easy to feel like something is medically wrong, which only makes the anxiety worse.
If you struggle with these physical alarms, you aren't "crazy," and you aren't broken. Your nervous system is simply working overtime. Here is how to understand those signals and respond to them without spiraling into panic.
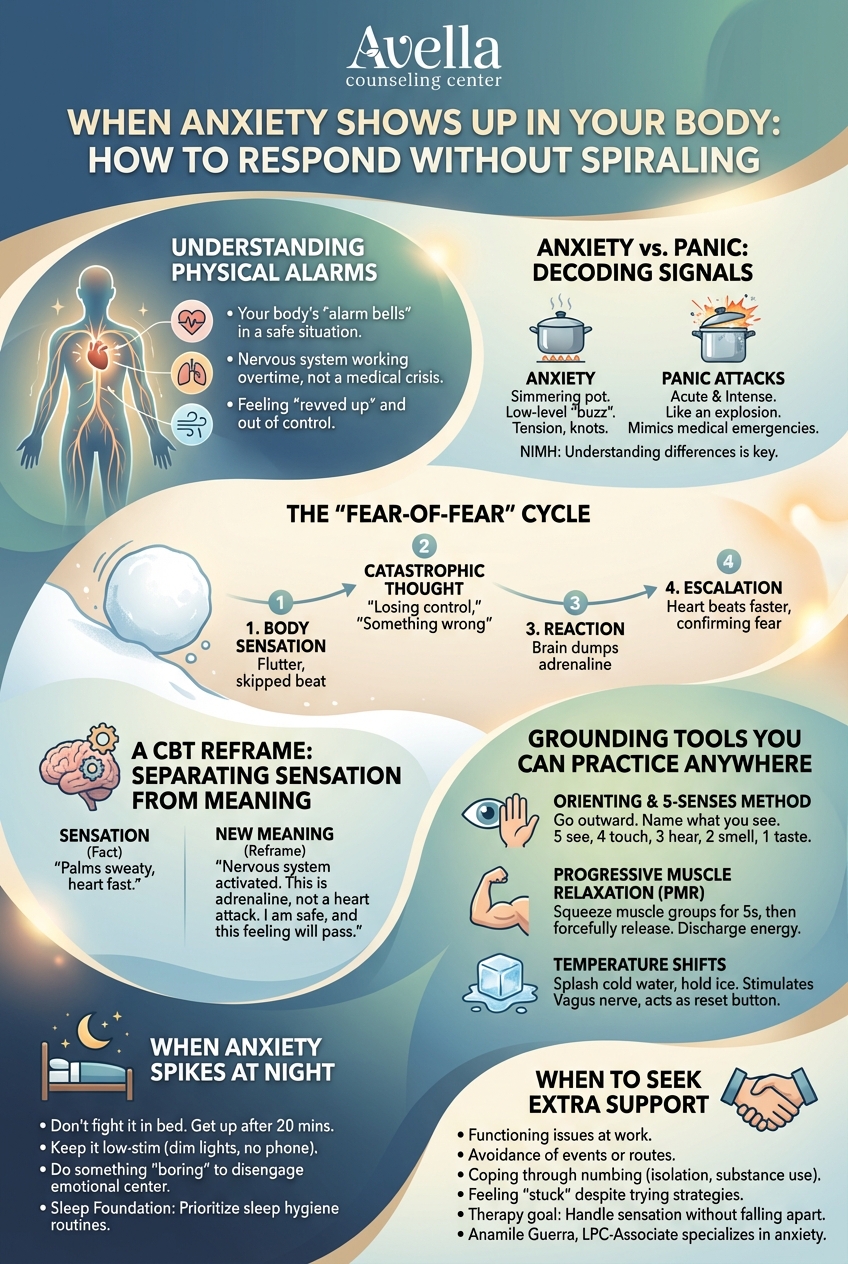
Anxiety vs. Panic: Decoding the Body’s Signals
It is important to distinguish between general high-functioning anxiety and a full-blown panic attack, though they often overlap.
- Anxiety often feels like a simmering pot. You might carry tension in your shoulders, feel a knot in your stomach, or have a low-level "buzz" of nervousness that lasts all day.
- Panic Attacks are acute and intense. They are the explosion. Symptoms often mimic medical emergencies: heart palpitations, dizziness, shortness of breath, and tingling in the hands.
It is incredibly common for people experiencing their first few panic attacks to end up in the ER or Urgent Care. You might see your blood pressure spike or your heart rate accelerate and think, "I’m having a heart attack." Once medical causes are ruled out, realizing these intense physical reactions are "just" anxiety can be confusing—but it is also the first step toward regaining control.
According to the National Institute of Mental Health (NIMH), understanding these differences is key to knowing how to treat them.
The "Fear-of-Fear" Cycle
Why do physical symptoms tend to get worse the more we focus on them? It’s often due to the fear-of-fear cycle.
Imagine a snowball rolling down a hill. It starts small—maybe a slight flutter in your chest or a feeling of heat in your face. If you ignore it, it might pass. But if your brain interprets that sensation as a threat, the snowball grows.
- The Body Sensation: You feel a skipped heartbeat or shallow breath.
- The Catastrophic Thought: You think, "I’m losing control," "I’m going to faint," or "Something is wrong with me."
- The Reaction: Your brain dumps more adrenaline into your system to "save" you.
- The Escalation: The adrenaline makes your heart beat even faster, confirming your fear that something is wrong.
This cycle can turn a minor uncomfortable sensation into a major panic episode.
A CBT Reframe: Separating Sensation from Meaning
One of the most effective ways to stop the snowball effect is using tools from Cognitive Behavioral Therapy (CBT). CBT helps us separate the sensation (what is actually happening) from the meaning (what we tell ourselves is happening).
When you feel that physical surge, try to pause and label the sensation neutrally.
- Sensation (Fact): "My palms are sweaty, and my heart is beating fast."
- Old Meaning (Fear): "I am about to pass out. This is dangerous."
- New Meaning (Reframe): "My nervous system is activated. This is adrenaline, not a heart attack. I am safe, and this feeling will pass."
Reframing puts a spoke in the wheel of those racing thoughts, giving your physical body a chance to catch up and cool down.
Grounding Tools You Can Practice Anywhere
Sometimes, clients tell me, "I tried deep breathing, and it didn't work." I validate that completely. When you are at a 10/10 level of panic, simple breathing can sometimes feel impossible or even suffocating.
If your nervous system is too elevated for breathing exercises, you need more active grounding techniques to signal safety to your brain.
1. Orienting and the 5-Senses Method
When we are anxious, we tend to go inward (focusing on the heart rate). To stop this, we must go outward.
- Look around the room. Turn your head and neck.
- Name what you see. "I see a blue chair. I see a wooden table."
- Engage your senses. Find 5 things you can see, 4 you can touch, 3 you can hear, 2 you can smell, and 1 you can taste. This forces your brain to focus on the external environment rather than the internal alarm.
2. Progressive Muscle Relaxation (PMR)
If you feel "stuck" or frozen, you might have excess energy trapped in your muscles. PMR involves squeezing your muscle groups (like making a tight fist or hunching your shoulders up to your ears) for 5 seconds, and then forcefully releasing them. This helps discharge that "revved up" energy.
3. Temperature Shifts
Splash cold water on your face or hold an ice cube in your hand. The sudden temperature change can stimulate the Vagus nerve, which acts as a reset button for your nervous system, slowing down your heart rate.
When Anxiety Spikes at Night
One of the most distressing forms of physical anxiety is waking up with a racing heart. You might wake up at 2 AM, heart pounding, with your mind immediately racing through worries about the past or future.
Because your defenses are down when you sleep, your brain creates a "fight or flight" response before you are even fully awake.
A Gentle Plan for Nighttime Anxiety:
- Don't fight it in bed. If you haven't fallen back asleep after 20 minutes, get up. Lying in bed tossing and turning trains your brain to associate the bed with stress.
- Keep it low-stim. Keep the lights dim and avoid your phone (blue light wakes the brain up further).
- Do something "boring." Read a dull book or fold laundry. This disengages the emotional center of your brain (the amygdala) and helps the logic center come back online.
- Prioritize Sleep Hygiene. The Sleep Foundation suggests consistent routines to lower overall cortisol levels before bed.
When to Seek Extra Support
It is normal to feel anxious occasionally. However, if physical symptoms are starting to run your life, it may be time to seek professional support. Signs that you might benefit from therapy include:
- Functioning issues: You are having trouble concentrating at work, re-reading emails constantly, or making mistakes because your mind is elsewhere.
- Avoidance: You are skipping social events, driving routes, or exercises because you are afraid of triggering a panic attack.
- Coping through numbing: You are turning to emotional eating, isolation, or substance use to "shut off" the brain.
- Feeling "Stuck": You’ve tried self-help strategies, but the symptoms persist.
In therapy, progress isn't about never feeling anxious again. It’s about feeling the sensation and knowing you have the tools to handle it without falling apart.
You Don't Have To Navigate This Alone
If physical anxiety is keeping you up at night or making you feel like you're losing control, support is available. You can learn to regulate your nervous system and reclaim your peace of mind.
Anamile Guerra, LPC-Associate (supervised by Jennifer Gonzalez, MS, LPC-S and Amanda Varnon, MA, LPC-S) specializes in helping clients navigate anxiety, stress, and self-esteem issues.





