Do you ever feel like your body is sounding an alarm, even when you’re trying to relax? Maybe it’s a stomach ache that won’t go away, a sudden loss of appetite, or a heavy fatigue that sleep doesn’t fix. You might go to the doctor expecting a medical diagnosis, only to hear, "Your tests are normal."
While hearing "it’s normal" should be a relief, it can often feel frustrating or confusing. If there is nothing medically wrong, why does it hurt?
As a therapist at Avella Counseling in Pearland, I often work with clients who start therapy discussing physical discomfort—like weight loss, nausea, or constant tension—before we ever get to the emotional triggers. We are not medical doctors, and we don't diagnose physical illnesses. However, we do help clients understand how the nervous system translates emotional stress into physical sensation.
If you are struggling with the physical symptoms of anxiety and depression, understanding the mind-body connection is the first step toward relief.
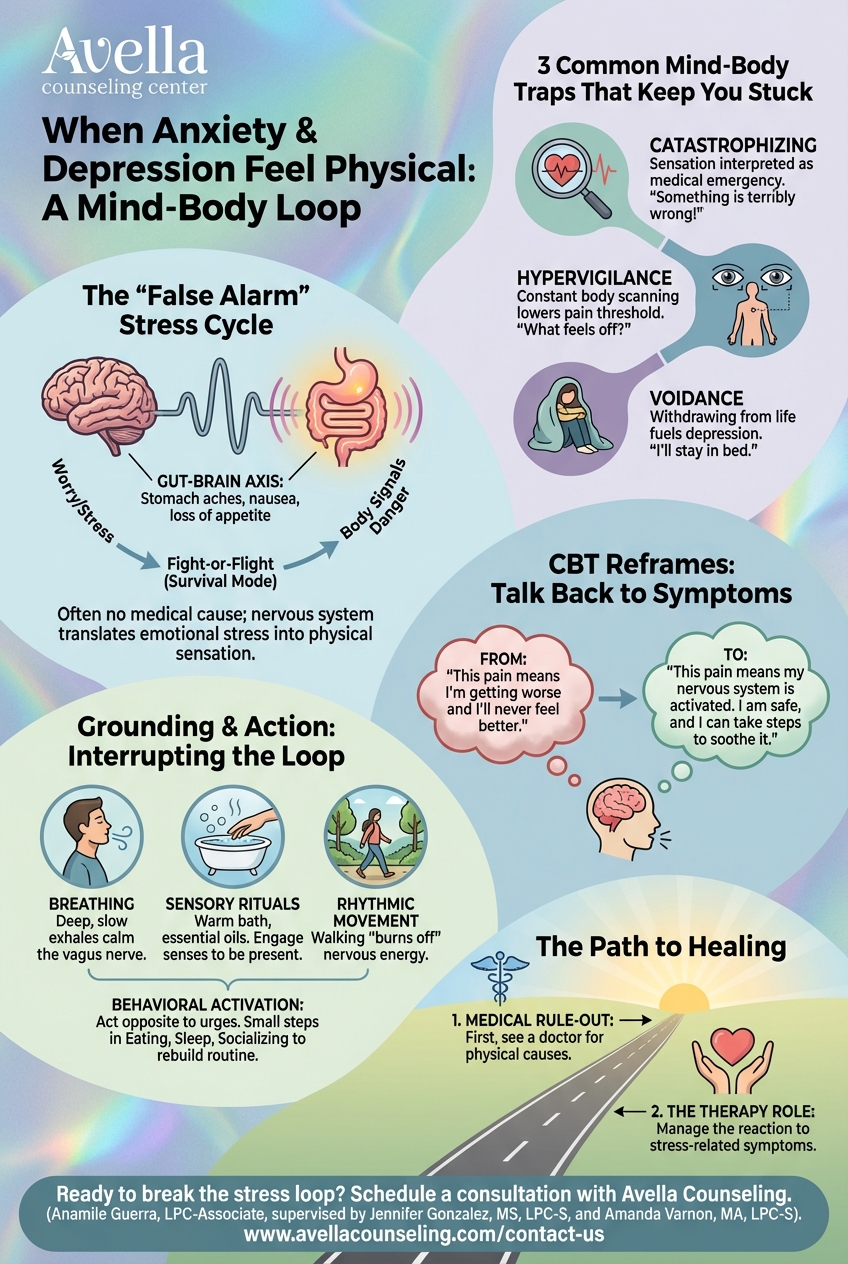
The "False Alarm": How the Stress Cycle Amplifies Sensation
When you are going through a period of intense worry, grief, or depression, your body often shifts into "survival mode." This is the fight-or-flight response. Your brain sends signals to your body to prepare for danger, even if the "danger" is emotional rather than physical.
One of the most common places this shows up is the gut-brain axis. Your stomach and brain are in constant communication. When your brain is stressed, it can slow down digestion, causing nausea, stomach cramps, or a complete loss of appetite.
I have seen clients who were so weighed down by grief and worry that they lost significant weight because eating felt physically painful. Their body was trying to protect them, but it got stuck in an "alarm" state. The good news is that by signaling safety to your nervous system, you can often reverse this cycle.
Learn more about the gut-brain connection from the Mayo Clinic.
3 Common Mind-Body Patterns That Keep You Stuck
Once the physical symptoms start, our reaction to them can sometimes make them worse. Here are three patterns we often address in therapy:
1. Catastrophizing (The "What If" Spiral)
This happens when you feel a physical sensation—like a fast heartbeat or a stomach cramp—and immediately interpret it as a medical emergency. You might think, "This pain means something is terribly wrong," rather than, "This pain is my body reacting to stress." This thought increases anxiety, which in turn increases the pain.
2. Hypervigilance (Body Scanning)
Anxiety can make you constantly scan your body for anything that feels "off." It’s like listening for a noise in a dark house; you will eventually hear something. When you are hyper-focused on your stomach or your breathing, you actually lower your pain threshold, making normal sensations feel intense.
3. Avoidance
When you feel sick or tired, the natural urge is to withdraw. You might stay in bed, skip meals to avoid stomach pain, or isolate yourself from friends. While this feels safer in the moment, it often fuels depression. We see clients who stop eating because of nausea, which leads to weakness and more fatigue, creating a difficult cycle to break.
CBT Reframes: Separating Sensation from Conclusion
In Cognitive Behavioral Therapy (CBT), we learn to talk back to these physical symptoms. The goal isn't to pretend the pain isn't real—it is real. The goal is to change what the pain means to you.
We work on shifting the internal dialogue from:
"This pain means I'm getting worse and I'll never feel better."
To:
"This pain means my nervous system is activated right now. I am safe, and I can take steps to soothe it."
I have witnessed clients who, after weeks of fearing their symptoms, realized that as they processed their emotions and stuck to a routine, the sharp pains began to decrease in frequency. Learn how to respond to body anxiety without spiraling.
Grounding Skills to Interrupt the Loop
When your body is loud, you need simple tools to quiet it down. Here are a few grounding techniques that can help:
- Breathing: Deep, slow exhales signal the vagus nerve to calm the heart rate.
- Sensory Rituals: Engaging your senses can pull you out of your head and into the present moment. For example, some people find great relief in "water therapy"—taking a warm bath with calming scents like herbs or essential oils. The warmth relaxes tense muscles, and the scent provides a new focal point for the brain.
- Rhythmic Movement: Walking is one of the best ways to metabolize stress hormones. It doesn't have to be power walking; simply being outdoors and moving at a steady pace can help "burn off" the nervous energy that sits in your stomach or chest.
Read more about a self-help reset you can use anywhere.
Behavioral Activation: Rebuilding Routine When You Don’t "Feel Like It"
Depression and anxiety often trick you into waiting until you "feel better" to do things. Behavioral Activation flips this: you do the things to help yourself feel better.
Rebuilding a routine when you feel physically ill from stress requires small, gentle steps:
- Eating: If you have lost your appetite, try small, bland meals (like toast, broth, or plain chicken) just to keep your fuel levels up.
- Sleep: Establishing a winding-down routine without screens.
- Socializing: Connecting with a community, faith group, or family member, even for a short time.
We often see that when clients force themselves to "act opposite" to the urge to isolate—perhaps by taking care of a grandchild or attending a church service—they find moments of relief from their symptoms.
Read about coping when life feels like autopilot.
When to Seek Medical Help vs. When Therapy is Key
It is vital to approach physical symptoms responsibly.
- Medical Rule-Out: Always see your Primary Care Physician (PCP) or a specialist (like a gastroenterologist) first to rule out medical causes for your pain or weight changes.
- The Therapy Role: Once medical causes are managed or ruled out, therapy helps you manage the reaction to the symptoms.
According to the National Institute of Mental Health (NIMH), digestive problems and headaches are common physical signs of depression. If your doctor says, "It's stress-related," that is where we step in.
Conclusion
Physical symptoms of anxiety and depression are valid and challenging, but they do not have to control your life. Healing is a process. It often involves a combination of medical support, better nutrition, movement, and processing the emotions that are keeping your body in alarm mode.
If you are in the Pearland, TX area and physical symptoms of stress are disrupting your life, you don't have to navigate it alone.
Ready to break the mind-body stress loop?
Schedule a consultation with Anamile Guerra, LPC-Associate, supervised by Jennifer Gonzalez, MS, LPC-S, and Amanda Varnon, MA, LPC-S. Together, we can find strategies to help you reclaim your calm.





